ARTEMIS
Effective reserve for outcome prediction

Outcome prediction is often seen as the 'holy grail' of medical image analyses. Once we are able to accurately predict the outcome of an individual patient, we are able to find the set of clinical variables, such as sex, age, hypertensive status, etc., which allows us to predict the disease progression. This in turn then enables early interventions and targeted therapy which will ultimately help us to improve patient's lives. However, outcome prediction is very challenging. Even if we look at two very similar patients, meaning from the same country, same age, same sex, similar lifestyles, have a stroke in roughly the same area of the brain, their outcome can be vastly different. This suggests that an underlying mechanism exists, which influences patient recovery, but which we are unable to identify and measure at this point.
In the second aim of this project, our aim is to characterize the remaining brain reserve of stroke patients. The full scientific publication is freely available here. Brain reserve represents in simple terms the capability of the brain to compensate for negative effects. Clinicians, for example, often observe 'patients' who do not exhibit any symptoms, however, demonstrate clear pathology in their examination. The big question then was, how do we describe this phenomenon? Brain reserve is rooted in the threshold theory, which states that brain pathology must reach a certain threshold before symptoms show, where this threshold can be patient specific. This can be visualized as a bucket in the brain which slowly fills up with water (reserve), until it overflows (symptoms show). The water in the bucket subsequently represents information on how many negative effects are already being compensated, such as advanced age, disease states such as hypertension, and potentially genetic contributions. Each new disease or insult then adds water to this buckets, where symptoms manifest themselves, once the bucket 'overflows'.

Generally, we can differentiate between two types of reserve; the structural/biological reserve and the functional/cognitive reserve. Cognitive reserve is based on the observation that, for example, higher education can be protective against neurodegenerative diseases, which might be seen as a muscle, which, through a 'workout', gets stronger, and subsequently increases the total reserve or capacity to compensate for negative effects. On the other hand, the brain reserve may get 'occupied' with each insult or disease a patient encounters. Ultimately, we are interested in the effective reserve, which is a term to describe the 'unoccupied' reserve left with which a new disease can be compensated.
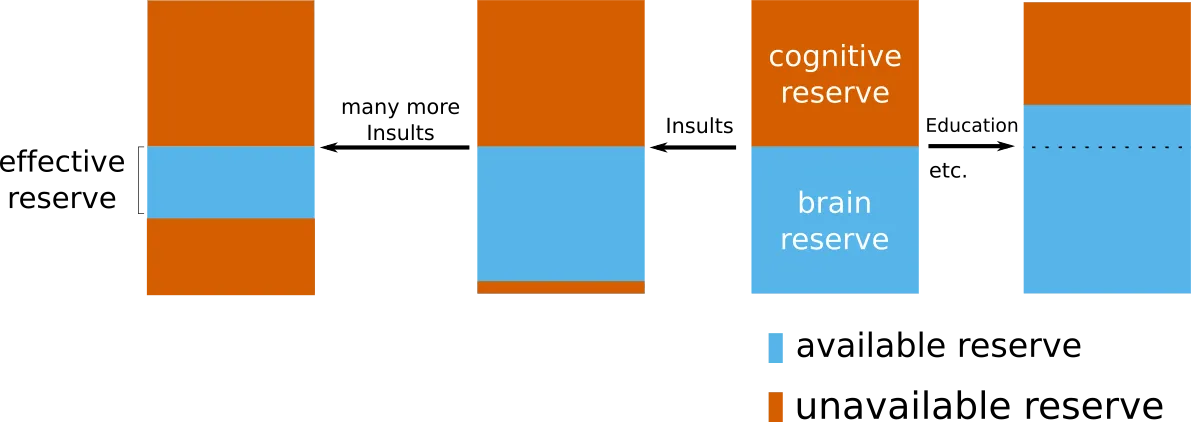
However, measuring effective reserve is difficult, considering we are describing a fuzzy concept that we do not fully understand yet. Nonetheless, by using latent variable models, we can start describing the effect.
Where there is smoke, there is fire.
Latent variable models are based on the idea that we can describe the 'fire' by looking at the 'smoke'. This means that we are using indirect measures of this latent variable to characterize it. In the literature, effective reserve, as it refers to the remaining brain reserve, is related to the brain volume of a person, where it is assumed that larger brain volumes relate to larger number of neurons. In addition, we already observe that the older a patient is, the less likely it is that a compensation of the negative effects is going to be successful. As we are working in stroke populations, we also included the assumption that the systolic blood pressure (SBP; the lower of the two blood pressure measures) at time of admission is related to the effective reserve. If the model of effective reserve is correct, we would expect to see a negative association between itself and the modified Rankin Scale (mRS) score, where lower values correspond to better outcomes (in simple terms, the higher the effective reserve, the better the outcome).
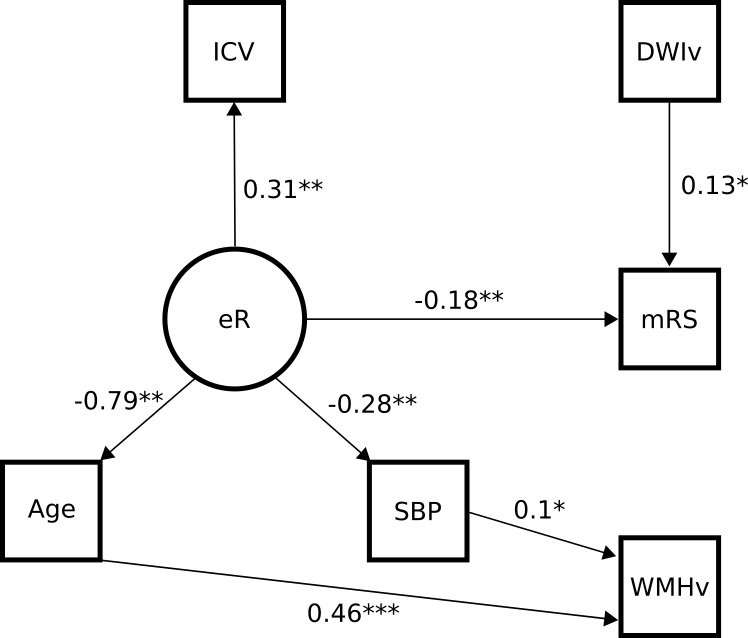
Utilizing the power from the Genes Affecting Stroke Risk and Outcomes Study (GASROS) study, which was started with the aim to genetic factors that contribute to stroke risk and outcome, of which a total of 453 patients were eligible for our investigation into effective reserve. The model, which includes effective reserve and was fit to the data can be seen in the figure above. Importantly, we did not included any directionality in the relationships (shown as small numbers on top of the arrows), which means, for example, that we did not specify that effective reserve should be associated with a positive outcome. However, our model indicates that intracranial volume (ICV), as a surrogate measure of maximum brain size over the life-span, increases effective reserve. Similarly we observe negative effects of age and systolic blood pressure on the remainder of the brain reserve, while reproducing known associations between age and white matter hyperintensity volume (WMHv), systolic blood pressure and white matter hyperintensity volume, and acute lesion volume (DWIv) and outcome.
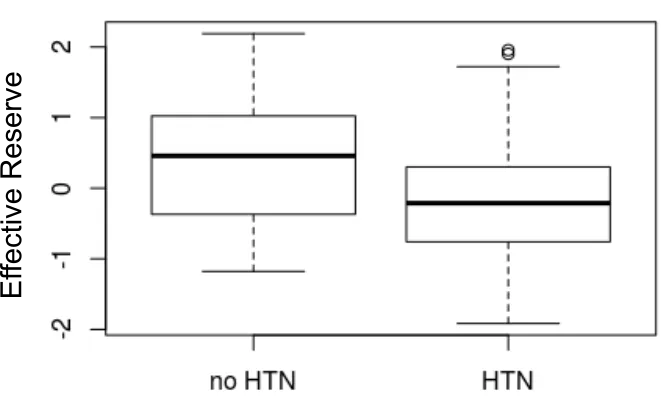
In an attempt to answer this question, we investigated if effective reserve might be related to vascular health, considering the patient population we are studying. In our population we had additional information on hypertensive (HTN) status, which we used as a proxy of the overall vascular health, under the assumption that better vascular health is present in those not exposed to long-term effects of hypertension (i.e., non-hypertensive patients). In this study, we saw a significant group difference, suggesting that non-hypertensive patients exhibit higher effective reserve. This means that effective reserve may indeed be representative of vascular health, however, future studies are necessary to confirm the vascular health theory. Nonetheless, we were able to show that effective reserve is related to better functional post-stroke outcome, which can help to create patient specific disease models and ultimately aid in the prediction of long-term patient outcome.